|
 Vitamin D functions within two systems in the human body: 1. The endocrine system - maintains calcium homeostasis and bone health. This system uses the metabolized form of vitamin D called 25(OH)D and by the time it is turned into 1,25(OH)2D, the usable form, it has a half life of three weeks. All the studies on bone health have been successful based on dosage, not frequency, because of this long half life. 2. The autocrine/paracrine system - vitamin D is delivered to non-skeletal systems such as breast, colon, and prostate tissues and helps affect autoimmune disorders, cancer, cardiovascular disease and infections. In this system, vitamin D goes into a cell and helps regulate cell growth, after this process vitamin D has a half life of 24 hours, meaning frequency of dosing matters when testing for disease reduction and immune control.
Interview Summary How is vitamin D absorbed and used in your body? Vitamin D3 enters the body through sun exposure, diet or a  supplement and goes into the blood stream where it binds to the vitamin D binding protein (VDBP) -- a protein that carries vitamin D compounds into circulation. From there, vitamin D3 functions within two systems in the human body (the two systems mentioned above?). supplement and goes into the blood stream where it binds to the vitamin D binding protein (VDBP) -- a protein that carries vitamin D compounds into circulation. From there, vitamin D3 functions within two systems in the human body (the two systems mentioned above?). The first is the endocrine system, which maintains calcium homeostasis and bone health. In this system, vitamin D3 is transported to the liver where it is metabolized into 25(OH)D. The 25(OH)D along with the VDBP complex (binding protein) is then transported into the kidneys via a special active transport system--called the megalin-mediated system. The kidney's enzymes transform the compound into the active hormone 1,25(OH)2D, and the kidney then excretes 1,25(OH)2D back into the blood stream where the intestine helps facilitate calcium absorption--maintaining bone health. The second of these systems is the autocrine/paracrine system. Through these pathways, vitamin D3 is delivered to the majority of non-skeletal systems such as the breast, colon, skin, brain, ovary and prostate tissues. While vitamin D3 is transported through the blood stream, it breaks its bind from VDBP and enters the body's various cells via simple diffusion. Within the cell, enzymes metabolize the vitamin D3 to 25(OH)D and then to 1,25(OH)2D, which works to regulate cell growth and perform other helpful functions. 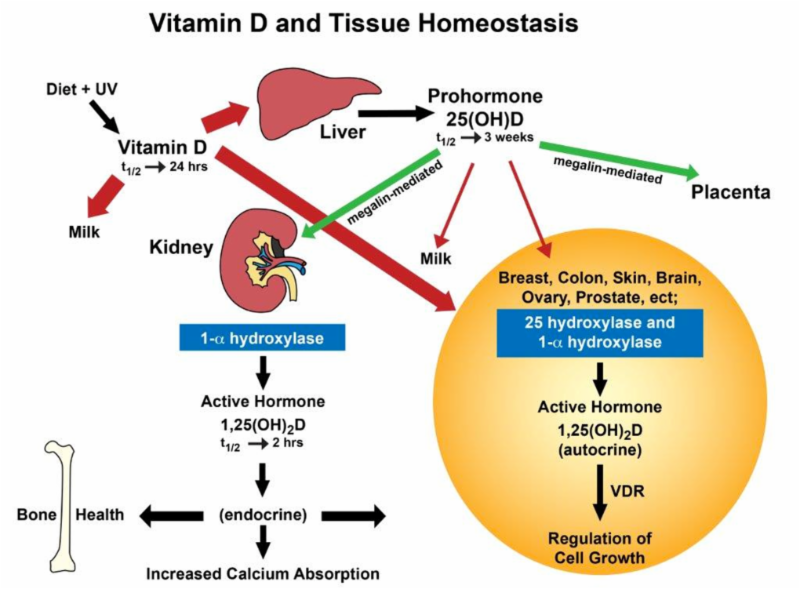 Tissues in the autocrine/paracrine system are not equipped with the megalin-mediated transport system, so if vitamin D compounds are bound to the VDBP, they cannot enter these cells. Vitamin D3 binds loosely to the VDBP and can easily break off and enter the cells of the autocrine/paracrine system. Conversely, 25(OH)D binds very tightly to the VDBP and only a small amount is able to break free and enter these tissues. Therefore, vitamin D3 is needed for these non-skeletal systems. Why is daily vitamin D input needed?  The length of time that a vitamin D compound stays in the blood is based on how tightly it is bound to the VDBP (the vitamin D binding protein). The 25(OH)D used in the endrocrine system has a half life of three weeks because it is bound very tightly to the VDBP, while vitamin D3 used in the autocrine system has a half life of 24 hours. Therefore, a daily input is needed to maintain stable vitamin D3 levels for non-skeletal systems. For bone health, a weekly or even monthly intake would have a positive effect on the body. The length of time that a vitamin D compound stays in the blood is based on how tightly it is bound to the VDBP (the vitamin D binding protein). The 25(OH)D used in the endrocrine system has a half life of three weeks because it is bound very tightly to the VDBP, while vitamin D3 used in the autocrine system has a half life of 24 hours. Therefore, a daily input is needed to maintain stable vitamin D3 levels for non-skeletal systems. For bone health, a weekly or even monthly intake would have a positive effect on the body.
For example, if someone takes a large dose of vitamin D3 on a weekly basis, within a couple days all of the vitamin D3 is metabolized into 25(OH)D, which cannot get into the cells.. For the remaining five days until the next weekly dose, the body would have no detectable vitamin D3. Do nursing mothers need daily D3?  Breast feeding mothers could have 50-60 ng/ml of measurable 25(OH)D in their blood but no measurable vitamin D3 in their breastmilk so dosing daily is important. After vitamin D3 has been turned to 25(OH)D it cannot enter the breast milk. The only way to get vitamin D in breastmilk is by dosing daily - either by sun, diet or supplementation. Dr. Hollis' research indicated that 6,400 IU/day was necessary for breast feeding mothers. Breast feeding mothers could have 50-60 ng/ml of measurable 25(OH)D in their blood but no measurable vitamin D3 in their breastmilk so dosing daily is important. After vitamin D3 has been turned to 25(OH)D it cannot enter the breast milk. The only way to get vitamin D in breastmilk is by dosing daily - either by sun, diet or supplementation. Dr. Hollis' research indicated that 6,400 IU/day was necessary for breast feeding mothers.
Why does this matter for clinical trials?  Most of the clinical trials conducted in the past 40 years have focused on the endocrine system and have consistently shown the positive effects of vitamin D on bone health regardless of dosing regimen (from daily to quarterly). In the past 10 years, many new clinical trials have focused on non-skeletal outcomes such as autoimmune disorders, cancer, cardiovascular disease and infections. These new studies have also used various dosing regimens--but have yielded inconsistent results. Those with adequate daily vitamin D inputs have largely shown positive results while those with longer dosing intervals have shown no vitamin D effect. While 25(OH)D levels are maintained in these studies, it is the vitamin D3 levels that are essential to these systems. Therefore, it is necessary to design a clinical trial based on the physiology of the system of interest in order to accurately assess the effect of vitamin D in the body. Most of the clinical trials conducted in the past 40 years have focused on the endocrine system and have consistently shown the positive effects of vitamin D on bone health regardless of dosing regimen (from daily to quarterly). In the past 10 years, many new clinical trials have focused on non-skeletal outcomes such as autoimmune disorders, cancer, cardiovascular disease and infections. These new studies have also used various dosing regimens--but have yielded inconsistent results. Those with adequate daily vitamin D inputs have largely shown positive results while those with longer dosing intervals have shown no vitamin D effect. While 25(OH)D levels are maintained in these studies, it is the vitamin D3 levels that are essential to these systems. Therefore, it is necessary to design a clinical trial based on the physiology of the system of interest in order to accurately assess the effect of vitamin D in the body.
Conclusion "Vitamin D intakes of up to 10,000 IU/per day and circulation 25(OH)D levels of up to 100 ng/ml (250 nmol) are normal in human physiology. Do not treat as poison." - Bruce Hollis |